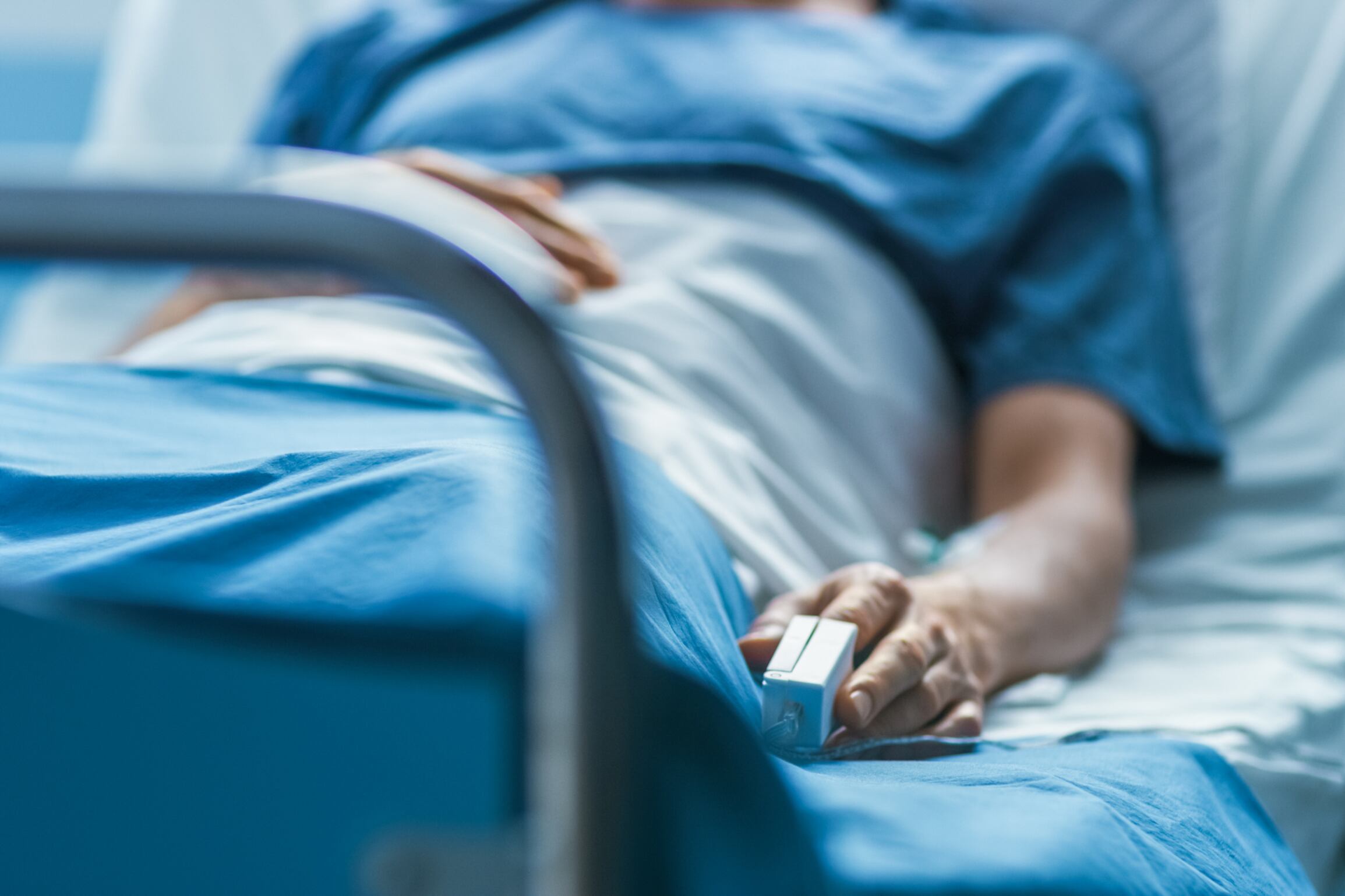
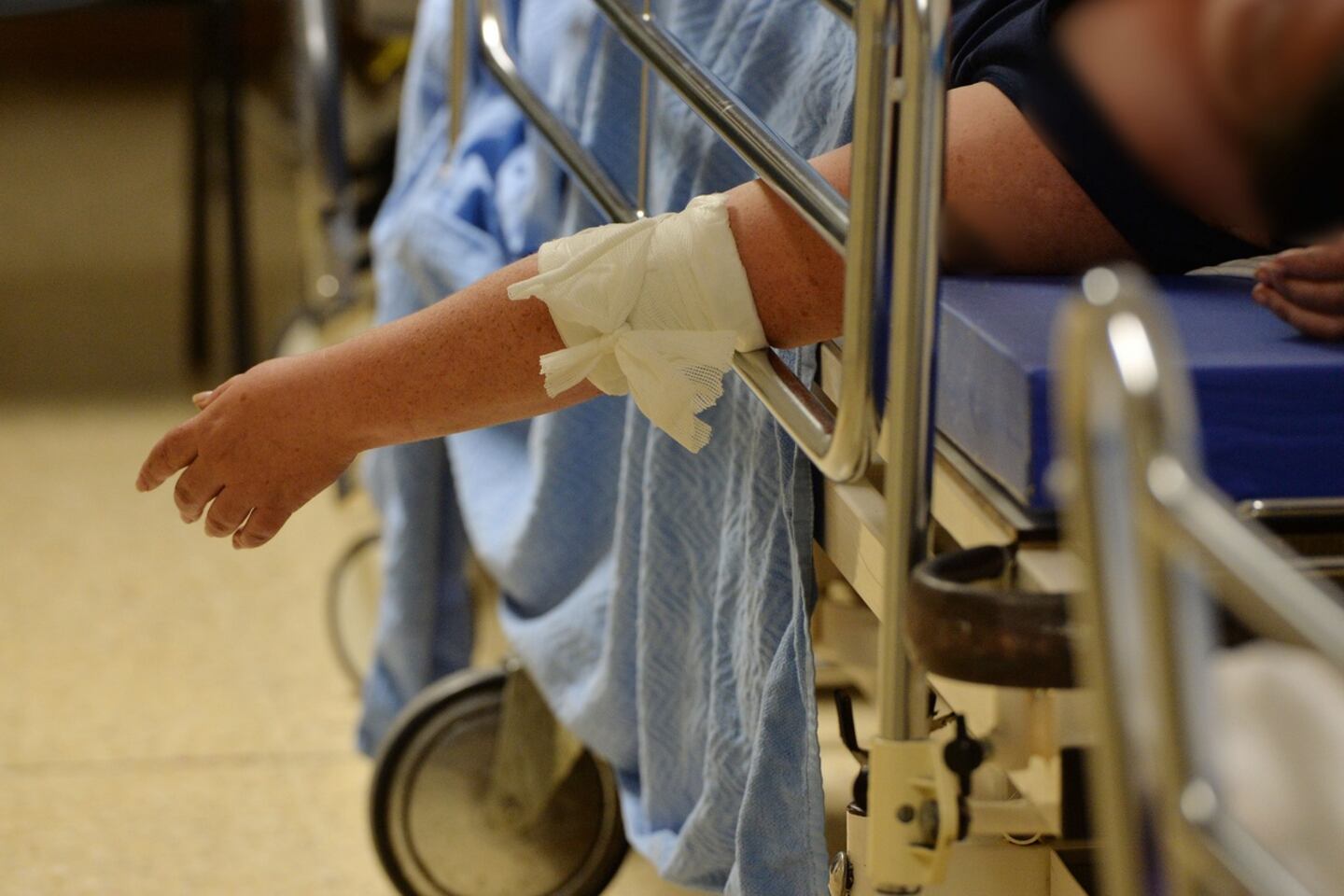
Large increases in healthcare funding and staffing in recent years has not been matched by a similar level of rising activity in Ireland’s hospitals, a significant new report has found.
The data, showing the growth in hospital activity is lagging considerably behind the level of State investment, is expected to be used by the Government to make the case for addressing productivity challenges.
The report drawn up by personnel in the Irish Government Economic Evaluation Service and the Department of Health says the health budget has risen from €13.7 billon in 2014 to €22.8 billion in 2024 and that more than 50,000 additional healthcare staff have been employed.
However, it says, “our analysis shows the large divergence present in all sites between the expenditure and workforce provided, relative to the growth in either separate activity metrics or ‘composite’ activity”. The latter is an aggregate for inpatient, day-case, outpatient and emergency activity, weighted by unit costs for each area.
RM Block
[ Hospital waiting lists may take up to a decade to clear, consultants warnOpens in new window ]
“In most cases, the divergence is significant, with the percentage growth in composite activity between 2016 and 2022 either negative, or two times behind workforce growth, and up to three times behind real expenditure growth over the same period,” the report says.
In a foreword, Department of Health secretary general Robert Watt and HSE chief Bernard Gloster describe the “identified divergence between resourcing and activity” as “a big concern”.
The report is to be published on Monday by Minister for Health Stephen Donnelly.
Part of the period covered by the report included the Covid-19 pandemic and it also acknowledged that not all hospital investment results in additional activity.
It says that between 2016 and 2022 there were increases in activity across all acute service areas (3 per cent inpatient complexity adjusted discharges, 10 per cent day-case complexity adjusted discharges, 20 per cent emergency department attendances, 2.6 per cent outpatient presentations).
“When we combine these based on their relative costs and adjust for the complexity of treatment, this equates to a 3.8 per cent increase in overall activity, compared to an inflation-adjusted rise in expenditure of 45 per cent (nominal rise of 68 per cent) and a 29 per cent increase in staffing numbers.”
On Monday Mr Donnelly will also unveil a new plan under which the health service will seek to generate savings of more than €500 million and introduce new reforms aimed at improving productivity.
It will look at making savings in non-pay areas such as on medicines, the procurement of items such as medical and surgical supplies as well as diagnostics and food.
[ Hospitals are getting more money but why is this not resulting in more activity?Opens in new window ]
The plan represents the initial work of a taskforce on savings and productivity established by Mr Donnelly in January.
It will seek to generate savings of €424 million in 2024 and more than €550 million in a calendar year. Other proposals may be added to the document at a later date.
The plan suggests a target of €20 million in savings on medicines this year as well as “actions to deliver increased savings in 2025 (including via inter alia enhanced best value medicine penetration rates, updating interchangeable lists, enhanced expenditure controls) across hospital and national schemes”.
It proposes savings of €34 million on reduced spending on external consultancies in the health service.
Under moves to drive efficiencies and boost productivity, GPs would refer patients to a team of specialists rather than to individual consultants as part of the introduction of “mandated central referrals per region per speciality“.
[ Government wants new children’s hospital to be open next yearOpens in new window ]
In relation to waiting lists it says there should be “mandated outsourced and technology enabled offerings where available to all people waiting more than 12 months who do not have an active plan” such as a project for remote consultations in the specialty of dermatology.
The plan also seeks to reduce the number of people who do not attend for scheduled appointments.
It suggests introducing “mandated patient-initiated reviews” in all appropriate settings for all specialities subject to the appropriate clinical qualifications. These involve a patient, caregiver or family member initiating an outpatient review appointment rather than the appointment being automatically scheduled.
The plan proposes new initiatives to avoid duplication of scans for patients ordered by both GPs and hospital doctors and the introduction of extra clinics and the maximum use of clinical infrastructure late evenings and Saturdays.
Meanwhile in advance of the publication of the new reports, the HSE said on Monday that a record number of patients were treated in hospital last year with the highest ever number of people receiving day-case care, attending outpatient appointments and receiving hospital care as inpatients.
- Listen to our Inside Politics podcast for the best political chat and analysis
- Sign up for push alerts and have the best news, analysis and comment delivered directly to your phone
- Find The Irish Times on WhatsApp and stay up to date